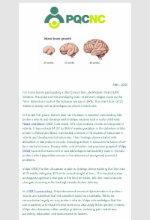
Late Preterm Infants
AAP Clinical Report - Late Preterm” infants: A population at risk (2007)
The purpose of this report is to define “late preterm”, recommend a change in terminology from “near-term” to “late preterm”, present the characteristics of late-preterm infants that predispose them to a higher risk of morbidity and mortality than term infants, and propose guidelines for the evaluation and management of these infants after birth.
AAP Clinical Report - Updates on an at-risk population: Late-preterm and early-term infants (2019)
This report discusses an increasing trend in LPI births since 2015. The report summarizes the initial progress of care for the LPI, discusses potential reasons for the current upward trend in LPI births and proposes research recommendations.
CPQCC Care and Management of the Late Preterm Infant Toolkit (2013)
This toolkit describes care planning, gestational age assessment, physiologic monitoring, education and evaluation of the late preterm infant.
WHO Recommendations for care of the preterm or low birth weight infant (2022)
This guideline includes 25 recommendations and 1 good practice statement for care of the preterm and low birth weight infant.
The Late Preterm - A population at risk (2018)
This article outlines the development of the LPI and common morbidities seen in this population. Discharge planning is discussed.
Late preterm infants - changing trends and continuing challenges (2020)
This article review recent trends regarding rate of late preterm births, common morbidities and long term outcomes with special attention to neurodevelopment outcomes.
Multidisciplinary guidelines for the care of late preterm infants (2013)
This article is largely written in table format outlining interventions for the healthcare team for each aspect of care for the late preterm infant and specifying corresponding parent and family education.
Bilirubin Monitoring and Management
AAP Clinical Practice Guideline Revision: Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation (2022)
This guideline updates and replaces the 2004 AAP clinical practice guideline for the management and prevention of hyperbilirubinemia in the newborn infant > 35 weeks gestation. The guideline addresses issues of prevention, risk assessment, monitoring and treatment.
AAP Technical Report: Diagnosis and management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation (2022)
This technical report updates the evidence base necessary to develop the 2022 AAP clinical practice guidelines for management of hyperbilirubinemia in the newborn infant > 35 weeks’ gestation.
Feeding and Nutrition for the LPI
ABM Clinical Protocol #10: Breastfeeding the late preterm (34-36 6/7 weeks of gestation) and early term infants (37 - 38 6/7 weeks of gestation), second revision 2016
The purpose of the protocol is to assist the LPI in breastfeeding to the greatest extent possible, heighten awareness of difficulties that LPI may experience with feeding, offer strategies to manage breastfeeding problems and prevent problems such as dehydration, hypoglycemia, hyperbilirubinemia and hospital readmission.
ABM Clinical Protocol #1: Guidelines for glucose monitoring and treatment of hypoglycemia in term and late preterm neonates, revised 2021
This protocol provides guidance on differentiation transitional hypoglycemia from persistent hypoglycemia, appropriate monitoring of blood/plasma glucose levels, management of clinically significant hypoglycemia, maximizing milk production and preserving maternal milk supply.
Nutrition in late preterm infants (2019)
A discussion of what to feed the late preterm infant, how to feed and supplementation with breastmilk and formula are included.
A prospective cohort study on lactation status and breastfeeding challenges in mothers giving birth to preterm infants (2022)
This article provides a scientific discussion of lactogenesis onset and breastfeeding, values predictive of expressed milk volume on day 7 postpartum and breastfeeding status at 3 months of age.
Feeding the late and moderately preterm infant: A position paper of the European Society for Pediatric Gastroenterology, Hepatology and Nutrition Committee on Nutrition (2019)
ESPGHAN performed a literature review with the aim of providing guidance on how to feed infants born late or moderately preterm, identify gaps in the literature and research priorities.
Nutritional support strategies for the preterm infant in the NICU (2018)
This article provides a deeper dive into the necessary nutrients for the late preterm infant via enteral and oral routes of feeding.
LATCH: A breastfeeding charting system and documentation tool (1994)
The original article from JOGNN describing the LATCH tool.
Nutritional policies for late preterm and early term infants - can we do better? (2019)
A discussion of recent trends with LPI births, challenges for nutrition of LPI including hypoglycemia, hypernatremia and hyperbilirubinemia, energy and nutrient requirements and breastfeeding support.
LATCH score as a predictor of exclusive breastfeeding at 6 weeks postpartum: A prospective cohort study (2018)
Study demonstrates the utility of LATCH scores in the first 48 hours after birth to predict exclusive breastfeeding rates at 6 weeks postpartum.
Low LATCH score: A red flag sign and an educational tool for intervention among mothers to promote exclusive breastfeeding (2023)
Study assessing LATCH score after delivery and within 24 hours, at 48 hours and at discharge. A LATCH score of less than 6 at 48 hours can be a significant indicator for intervention to promote exclusive breastfeeding.l
Safe Sleep Practices for the LPI
AAP Updated 2022 recommendations for reducing infant death in the sleep environment
Improving hospital infant safe sleep compliance by using safety prevention bundle methodology (2021)
Performance improvement project utilizing a hospital wide safe sleep bundle and a safe sleep performance improvement team utilizing standardization of the infant sleep environment education.
Steering the Titanic: One tertiary care children’s hospital’s experience navigating safe sleep for hospitalized infants (2023)
A quality improvement project to improve compliance with safe sleep practices, documentation of infant sleep position and environment every shift and documentation of caregiver education.
Improving safe infant sleep compliance through implementation of a safe sleep bundle (2022)
A quality improvement project to implement a safe sleep bundle and evaluate its effective in improving caregiver compliance to safe sleep practices in a level III NICU.
Modeling safe infant sleep in the hospital (2020)
This quality improvement project evaluated a staff education intervention using a pre and post design. Noncompliance with known safe sleep practices was observed by providers demonstrating a need for continued education regarding safe sleep practices.
Mother’s decision making concerning safe sleep for preterm infants (2021)
Mixed-methods design study to identify factors influencing mothers’ decisions regarding sleep practices of LPI. Themes identified included adherence to safe sleep recommendations, nonadhereence to safe sleep recommendations and infant guided decisions.
Discharge of the Late Preterm Infant
Discharge Criteria for the Late Preterm Infant: A review of the literature (2017)
Provides a discussion and list of standardized discharge criteria for the late preterm infant. A checklist format is included.
Neonatal management and safe discharge of late and moderate preterm infants (2012)
The article discussed special challenges of transition and thermal adaptation, nutritional compensation for postnatal growth restriction, establishment of early feeding and avoidance of post-discharge jaundice or apnea.
Variation in Car Seat Tolerance Screen Performance in Newborn Nurseries (2020)
This article outlines a survey conducted of 84 NBN utilizing the BORN network to determine what percentage of NBN perform car seat tests on infants, inclusion and failure criteria, performance characteristics, follow up of failed car seat tests including the use of a car beds and provider attitudes towards car seat testing.