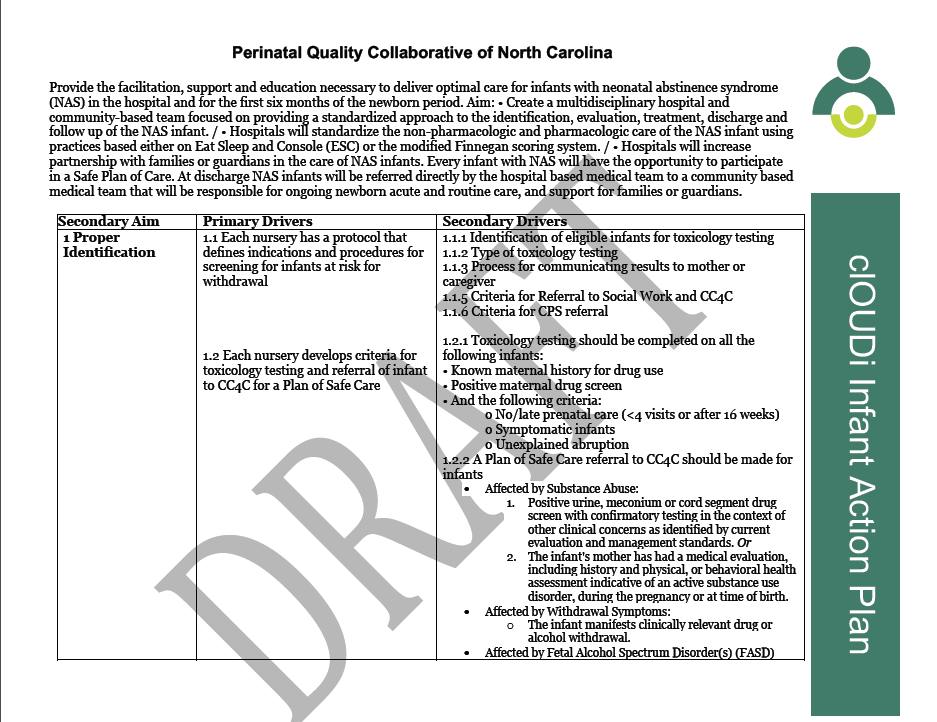
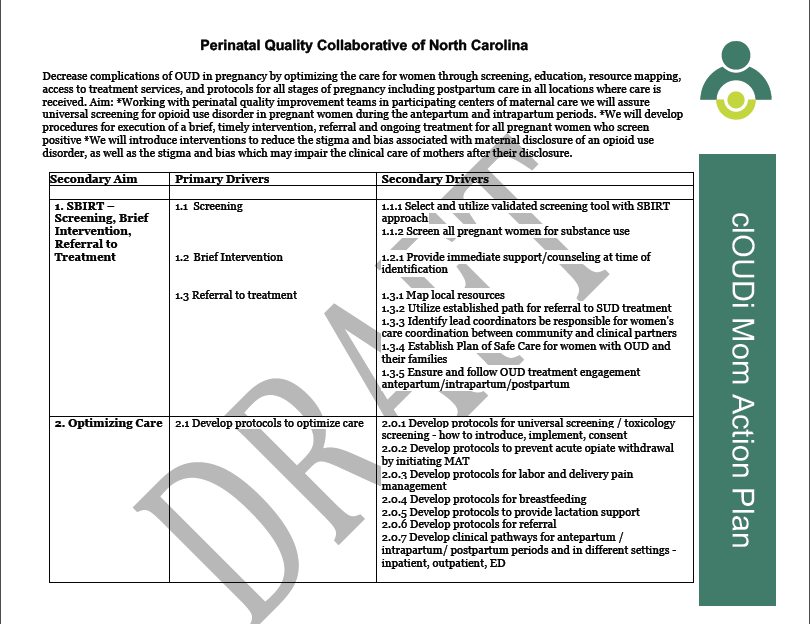
We are looking forward to the creation, development and then execution of our next project, a combined effort that will focus on Maternal Substance Use and Neonatal Abstinence Syndrome. This initiative will for the first time engage PQCNC in work that requires specified activities in the pre and post-partum periods. Similarly we will be planning interventions to support the care of newborns born to mothers living with substance use disorder.
Meetings for the Expert Team that will develop the AIM statement, key driver diagram and metrics for this project will begin in January 2020. Launch for this initiative will be January 2021. If you have experience, knowledge, expertise or interest in supporting the creation of such an initiative, please join us. We are calling on mothers, fathers, family members, docs, nurses, therapists, social workers, counselors, hospital and clinic leaders, addiction specialists, midwives, practitioners, public health officials, government leaders, and payers/purchasers of healthcare to consider joining us.
The only requirement for "Expert" is a willingness to read background materials we supply and commitment to joining us for perhaps one face to face meeting and 4 webinars over 6-8 months.
This is an initiative that is critically needed. We have all been touched in different ways by this growing crisis. Please join us in developing an initiative that will allow us to address how we make North Carolina the best place to give birth and be born for families living with maternal substance use disorder.
To join the Expert Team please click here